Throughout the past two years, there has been an emphasis placed on the role of patient health care data, but more specifically, clinical data, in the development of new drugs and treatments and the personalization of care. When leveraged properly, the insights within clinical data can close gaps in care, help achieve health equity, and ultimately improve patient health outcomes.
As the role of clinical data becomes more prominent, patients’ knowledge of how health care data is being used becomes more relevant. Q-Centrix is keenly aware of these broader uses and seeks to uncover patients’ attitudes and beliefs toward the sharing of their health care data and where education can be improved to help patients understand how their clinical data contributes to the advancement of medicine. For that reason, Q-Centrix commissioned its first Health Care Data Sharing Survey of 1,191 Americans in December 2021.
Notable findings from the survey include:
- When asked what types of data are collected and shared, the majority of respondents chose the typical information used in marketing initiatives, including personal (name, address, phone, etc.) (87%), demographic (74%), and location tracking (73%). Just over half of respondents (52%) selected health information.
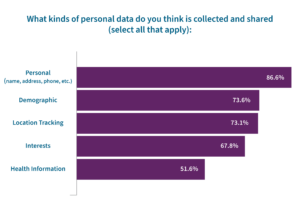
- However, while more respondents reported being very concerned (42%) or somewhat concerned (45%) about their personal data being shared, there was less concern around how health data is shared, with 35% reporting being very concerned and 39% being somewhat concerned.
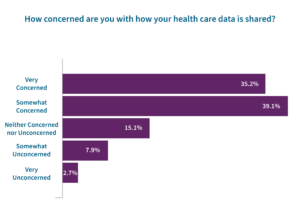
- While there is plenty of information about how personal data is used in marketing initiatives, it’s quite the opposite for health data, considering 61% of respondents indicated they have never discussed how their health care data is used.
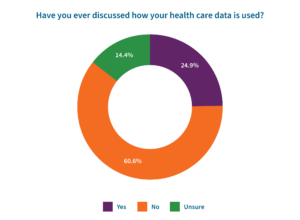
- Yet, despite not having a complete understanding of how health data is used, only one-in-five (22%) believe that sharing health care data is not important.
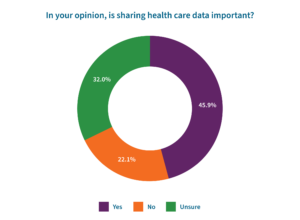
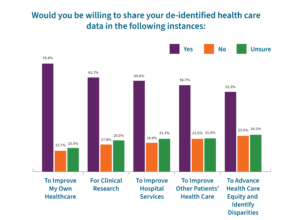
- This gap in knowledge of health data’s role in the health care industry becomes more apparent in willingness to share de-identified health information for purposes other than improving their health care. More than one-in-five respondents reported being unsure if they’d be willing to share their de-identified health care data for clinical research (21%), to improve hospital services (22%), to improve other patients’ health care (22%), and to advance care equity and identify disparities (24%).
- Moreover, one-in-four respondents report being unsure if they’re comfortable with their de-identified electronic medical records data/claims data being shared for patient care and research purposes, and one-in-three (33%) report being unsure if the widespread use of health care data is beneficial in achieving equitable health care.
With the health care industry’s growing reliance on electronic health records and medical claims to support regulatory decision-making for new treatments, these findings highlight an opportunity to improve patient understanding of the critical insights within their health care data and how the proper sharing of this data can help achieve public health objectives. The sharing of health care data allows clinicians and scientists to receive a full view of a patient, including disease stage, histology, comorbidities, past treatments, lab results, and more. This may translate into more effective care and improved representation in medical research and clinical trials.
A key part of this is assuring patients that their data is accurate and handled safely and securely. According to the survey, 35% of respondents do not believe the data recorded in their electronic medical record is accurate, and more than one-in-three are unsure (35%) or do not believe (37%) that organizations are doing everything possible to ensure their health data is protected. This also means being transparent about which organizations their data could be shared with, considering that most respondents (71%) only feel comfortable sharing their health care data with providers, hospitals, or pharmacies that have treated them directly.
“Hospitals have an opportunity to educate their patients on how they ensure their data is accurate and why that is important for improving outcomes,” said Brian Foy, Chief Product Officer at Q-Centrix. “This dialogue becomes even more prevalent as hospitals and health systems continue assessing patient consumerism and providing them with access to their health records and data. This not only requires clinician transparency but also the implementation of modern data solutions throughout hospitals and health systems to maintain data quality and security.”
Bridging this health care data knowledge gap will prove fundamental to the future of health care, which relies on real-time data for new treatment modalities and drugs. With proactive efforts to engage and educate, the health care system can take one step forward in innovating health care for all.